The McAndrews Method
JUMP TO:
INFORMED DECISION
ARTFUL PRECISION
UNPARALLELED RESULTS
Informed Decision, Artful Precision, Unparalleled Results
It is a matter of what we do, what we don’t do, and the person who does it. Our guiding philosophy is one that follows nature as closely as possible to elevate innovation to a living art form, creating an effect that doesn’t look like a hair transplant at all.
The McAndrews Method achieves four goals vital to a successful transplant:
- A result that’s as natural as possible and virtually undetectable
- Deliver the highest rates of survival and growth
- Create a result that looks great now and later
- Performs a transplant that’s conservative in technique, incredible in result
INFORMED DECISION
Know What to Expect: The Basics
Quite simply, a hair transplant is a process in which we take hair from the areas where you have more, then carefully and artfully transplant it where it’s needed. Requiring anywhere from four to eight hours, this is a procedure that is proven and natural-born when in the right hands. While the fundamental process is the same, every surgeon makes many choices and utilizes specific and very different techniques. Everyone makes a significant impact in how successful your hair restoration will be, and that makes your decision anything but simple.
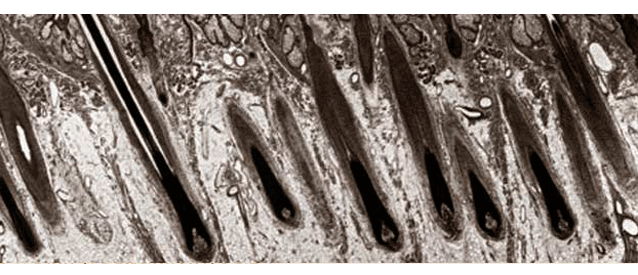
Q: Where does donor hair come from?
A: Male and female patterned hair loss is secondary to genetics and the hormone Dihydrotesterone (DHT). While hair on the top and front of the head is susceptible to the thinning effects of the DHT hormone, hair on the sides and back of your head isn’t. We use these areas where you have more hair to act as a “hair bank” for those where you don’t.
Q: How do I know if I’m a candidate for a hair transplant/ hair restoration?
A: While an office visit is absolutely essential to answer this question, the short answer is most men and women with realistic goals can get great results. Your age and the extent of your hair loss are also very important factors. Getting a hair transplant too young or when you’ve just begun noticing hair loss is unwise. Your hair loss pattern can change significantly and alter the effect of a hair transplant’s placement strategy. A premature hair transplant procedure may be outgrown as time passes and loss progresses.
Q: What about the hair loss pattern?
A: Again, hair loss will continue and threatens the longevity of your hair transplant’s natural effect. Typically, the average male patient loses approximately 4% density each year. For example, a 30% density will be decimated to 10% within 5 years, yet hair transplanted areas will remain the same. It’s imperative that every hair transplant is designed with this in mind, and not simply filled in for an instant gratification that expires quickly.
Q: How do I know if my hair transplant goals are realistic?
A: Only by having a thorough consultation with an experienced, formally trained physician. Of course, every patient should expect and demand completely natural results. The primary limitation to hair transplantations is that every patient has a fixed and limited amount of “good genetic” hair that can be transferred to the thinning area. A patient with more extensive hair loss may not be able to maintain a “full head of hair look”, however it still should look completely natural.
Q: Why is it important to understand this limitation of hair transplants?
A: Understanding this limitation and how it applies to your particular degree of hair loss is crucial to determining if you have realistic expectations and is really one of the most important factors in making an informed decision about your treatment options.
Q: How many hair transplant procedures are needed?
A: There is no preprogrammed answer to that question. Determining factors include:
- Existing density and the target density
- Rate of continued hair loss which can be drastically slowed by medical therapies like finasteride (Propecia) and minoxidil (Rogaine)
- Personal preferences, which can change over time.
Therefore, some patients only need a single hair transplant. Others need one hair transplant today and return in two or twenty years to fill in where nature and destiny have taken action. Even concurrent procedures should be timed no sooner than every 9-12 months. This allows each hair transplant to achieve its full result, as density improves over time.
A premature hair transplant procedure may also damage some previously transplanted hair that isn’t given the chance to reach its potential. Since The McAndrews Method leaves virtually no visible scarring in the recipient area (the thinning area), there’s no way to pinpoint exactly where new follicles may be getting ready to go to work.
Q: Will it keep growing?
A: Yes, thanks to a phenomenon called “donor dominance” transplanted hair always grows as well as it did in its area of origin. The only vulnerabilities are damaged follicles or poor transplantations, and our method virtually eliminates those risks.
Q: Are the medical therapies necessary?
A: Hair transplants fill in areas of baldness or thinning but they cannot stop the progressive nature of hair loss. Only the medical therapies, Propecia (finasteride) and Rogaine (minoxidil), can slow and stop the progression of hair loss. While many doctors do not encourage the use of these medical therapies in conjunction with hair transplants, The McAndrews Method advocates them. You should use every weapon in your arsenal to prevent further hair loss, which ultimately may benefit the patient by minimizing the need for future hair transplant surgeries.
ARTFUL PRECISION
Designing the Hair Line
The best hair transplant doesn’t look like one at all. The way to achieve it is by following the example of nature itself. The McAndrews Method respects hair—its tendencies, its integrity and its inherent design. It’s a more exacting process with the rewards of incredible survival rates and the most natural-born effect possible.
The McAndrews Method is founded on the talents of an aesthetic surgeon’s skillful hand. However, that doesn’t mean that artistry overrules the artistic genius of nature. It mandates to follow hair’s own patterns for the best possible result in design as well as execution. It follows what nature intended before it got interrupted. The result? A naturally restored head of hair.
Q: What are the most important factors in designing the hairline?
A: Hair restoration is as much art as science, although many physicians value an automated technique, or speed, over aesthetics. The goal is to frame your face and maintain a youthful appearance that’s true to you, including your own growth/loss patterns. There are four key points:
Strategic Height
Unfortunately, hair loss does not stop with a hair transplant. Placing the restored hairline too low virtually guarantees you’ll outgrow it. True, placing it low is tempting, especially to younger patients. Yet a few years of hair loss later and the natural balding pattern reasserts itself, leaving an unnaturally bold hairline without enough good genetic hair to fill it in. The McAndrews Method uses a conservatively placed hairline that looks good now—and in 20 years.
Natural Lateral Balance
Too wide of a frontal hairline creates the very result you want to avoid, evoking a comb-over or hair piece look.
The Angle of Hair to the Scalp
Hair angles more acutely at the front of the hairline. Incisions are too often placed perpendicular to the scalp, which covers it poorly and looks obviously fake.
Irregularity
A straight, symmetrical hairline doesn’t exist in nature, which is why it attracts unwanted attention. The McAndrews Method will follow the tendencies, textures and growth pattern of your own hair. That means it’s naturally irregular, not overly linear or harsh.
As Nature Intended
Each and every hair doesn’t grow individually from the scalp. They grow naturally in groups of 1 to 4 hairs. One of the most important innovations in hair restoration was the discovery of these natural hair groupings. Rather than destroying these natural groupings for the sake of convenience, we fight nature with nature by following the scalp’s inherent design. Unfortunately, the FUE technique of hair transplants inherently causes more trauma to the natural hair groupings which affects the results.
Again, we follow nature’s plan in how we harvest, place and implant the hair grafts, ensuring the most natural look and an overwhelming rate of survival and success.
Supply & Demand
As we mentioned, there’s one significant limitation to any hair transplant: the amount of “good genetic” hair. One of the most important aspects of the artful precision with The McAndrews Method is that we use this limited supply as wisely and efficiently as possible to meet the hair loss demands.
Preserving, placing and encouraging its growth are key components of The McAndrews Method. We use only techniques and technologies that ensure transplanted hair grafts survive and thrive without damage or depletion. The result? A naturally restored head of hair.
Q: Is there a difference in the hair grafts?
A: Absolutely. The McAndrews Method takes advantage of these natural hair groupings. Carefully and precisely. By maintaining this integrity, the look is far more natural and the survival is far greater than popular single-hair micrografts. That technique dissects only individual hairs, despite this inherent plan. Unfortunately, FUE hair grafts significantly increases the trauma to the natural hair groupings.
Q: How do you identify the natural hair groupings?
A: Critical to The McAndrews Method is another innovation—the “stereoscopic microscope” to identify these groupings with accuracy and dissect them with the utmost integrity. Without it, you’re seriously risking one of your most precious commodities: viable donor hair.
The microscope allows the doctor to precisely dissect the grafts, locating each unique grouping. This precision also prevents trauma to the surrounding hair. The result? The highest quality grafts with a dramatically higher success rate—95 to 100 percent. These results are typical for the McAndrews Method but are not the medical standard.
Note: During the critical dissection process, imperative to The McAndrews Method, is the use of the stereoscopic microscope. It is not “for show”. Using the stereoscopic microscope is the correct way to precisely dissect out each and every graft, which is the only way to ensure the best results for the patient. Unfortunately almost all doctors performing FUE hair transplants do not use or know how to use the stereoscopic microscope.
Q: Does this technique have other advantages?
A: Yes. The McAndrews Method of using the stereoscopic technique does have another important advantage: density. With the microscope, we can remove excess tissue from the hair follicle. That means your incisions are smaller, and smaller grafts can be placed more closely for a fuller, thicker effect. This is why it is still imperative to use the stereoscopic microscope even with an FUE hair transplant.
Q: How are the natural hair groupings placed?
A: The hairs that are naturally single get placed at the hairline. This careful placement is supported by multiple groupings placed farther back, designed for a thick appearance. The McAndrews Method of side-by-side placement of naturally grouped hair creates a lush, born-with-it density. And isn’t that what we’re all looking for? The stereoscopic microscope is useful to identify the size of the natural hair grouping in a FUE hair transplant in order to ensure larger grafts are not inadvertently placed on the hairline. Other methods of hair restoration place hair in straight rows in a line formation from front to back which is unnatural. Many times, bigger grafts are placed on the hairline when FUE hair transplants are performed without the use of the stereoscopic microscope.
UNPARALLELED RESULTS
The McAndrews Method Essential Attributes
What makes us different? Four essential qualities that are the best path to your most successful outcome. The McAndrews Method, by definition, implies each attribute is applied by the doctor—hands-on.

1. Technologically Advanced
We employ the latest techniques and technologies to maximize graft growth rates. To date, the stereoscopic microscope and natural hair groupings methodologies are unparalleled for highest possible success with both FUE and FUT hair transplant. As technology changes with the times, rest assured Dr. McAndrews, as a Clinical Professor at USC School of Medicine, remains on the cutting edge of all medical and surgical advancements in the field of hair loss.
2. Integrity
Patient first. All of our medical and cosmetic decisions are based upon what is best for the patient. If a hair transplant or particular technique is not in the patient’s best interest, it should not be performed. Sometimes this means going against the patient’s wishes.
3. Training
The McAndrews Method calls for any physician who performs hair transplants to be formally trained in both the medical specialty of dermatology (the experts in hair loss) and, more importantly, in the surgical art of hair restoration. Anything less is not sufficient to ensure a good result. (Most hair transplant facilities offer services headed by doctors of various specialties that have no formal training in the surgical art of hair restorations. BEWARE, recently many untrained doctors are illegally allowing unlicensed technicians to perform the FUE surgery with neograft, smartgraft, or other automated FUE device).
4. Expertise
These techniques are complex. The McAndrews Method ensures an expert in his field, as acknowledged by being a faculty member of a major teaching university, is doing your surgery. If a physician is not skilled enough to teach this art to others, why trust your surgery to him? There are perhaps a “hand-full” of doctors in the world that possess all of these attributes. However, even if they are the “apparent standards” of a physician, if a technician is the substitute for each critical phase of the procedure, then it is not within our guidelines. The McAndrews’ Method specifically calls for the physician with these attributes to apply them personally.
What don’t we do?
From risking donor hair to rushing surgeries, creating harsh hairlines to surgical shortcuts, there are many things our patients never need to worry about. The McAndrews Method stands apart from other providers for one very notable reason: Dr. McAndrews’ personal hands-on approach, performed each day with the utmost expertise, technique and integrity. In addition:
- We do not have technicians perform the majority of the hair transplant unsupervised. Dr. McAndrews is trained in hair restoration and is involved in every step of the process, never leaving the patient’s side throughout the surgery.
- We do not perform 3-4 hair transplants a day. Performing only one per day, we assure the doctor’s focus is that patient and only that patient.
- We do not perform single hair micro-grafts. This common practice takes individual hair grafts that destroy natural hair groupings—and with them, the precious resource of donatable hair. A Journal of Dermatologic Surgery study indicated this risky technique damages both the overall quality of grafts and their survival rates.
- We will not transplant irresponsibly. The most important role of physician is that of advisor. The oath of “first do no harm” leads us to advise patients unsuited to transplants against the surgery. Your long-term satisfaction is worth more to us than surgical fees.
- We do not rely on surgery alone, applying the medical treatments finasteride (Propecia) and Rogaine (minoxidil) are useful as additional tools in successful hair restoration
Finally, the most striking difference with The McAndrews Method is that I perform every procedure personally—just 1 per day to ensure undivided attention and unequaled care. Also, as a Clinical Professor at USC School of Medicine, I have mastered the latest advances in hair loss procedures and transplantations and bring them to my patients. It shouldn’t be any other way, because you deserve nothing less.
— Paul J. McAndrews, M.D.

*Model is an actual patient
Feel at ease with
your own hair.
Welcome to Dr. McAndrews’ Practice. Feel at ease that you are with the expert who trains other doctors with the latest advances in hair transplants. We are at the forefront of hair transplant, corrective hair transplant surgery, and medical hair loss treatment technology. We are dedicated to giving our patients the best hair restoration results with the highest level of service and care.








Our Locations in Los Angeles
Beverly Hills
435 N Roxbury Dr,
Beverly Hills, CA 90210
Pasadena
50 Alessandro Place, Suite 115, Pasadena, CA 91105
The McAndrews Method:
Informed Decision, Artful Precision, Unparalleled Results.
Dr. McAndrews' sole focus on his patients enables him to artistically and precisely create the best natural-looking results.
Get In Touch
If you have any further questions or would like to schedule a consultation, please do not hesitate to call or email us. You may also fill out the form provided to request more information.